Medical simulation allows the acquisition of clinical skills in a safe and protected environment. A trainee can make mistakes and learn from them without the fear of harming the patient.
Traditionally, medical simulation focused on training medical professionals to reduce errors, and optimize behavior during crisis – mainly in the field of emergency medicine and anesthesia. Throughout the years, the focus of medical simulation expanded into surgical simulation, training and optimization of soft skills (communication, leadership, teamwork etc.), general medical practice, as well as practical teaching into basic science such as anatomy and physiology.
The quality of the teaching experience may vary significantly, and depends on the pre-defined objectives, expertise of the tutors (incl. methodology), as well as the situational environment (e.g. type of simulators). Up to date, there is little standardization in simulation methodology, affecting further the quality of teaching. As described by Issenberg et al (2002), simulation is a deliberate practice involving (a) repetitive performance of intended cognitive or psychomotor skills in focused domain, coupled with (b) rigorous skills assessment, that provides learners (c) specific, informative feedback, that results in increasingly (d) better skills performance, in a controlled setting.
There are different types and classification of simulators, classified by their resemblance to the reality, or ‘fidelity’.
LOW FIDELITY
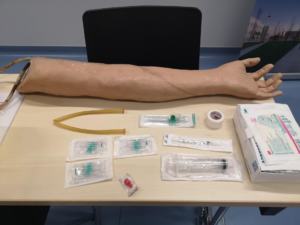
Task trainers to build specific skills, e.g. cannula or tube insertion, basic CPR skills. Lack realistic outlook and situational context: best for repetitive tasks as a first step for novices into technical skills.
An example of a skill trainer. Students can learn how to insert a peripheral inserted central catheter (PICC line)
MEDIUM FIDELITY
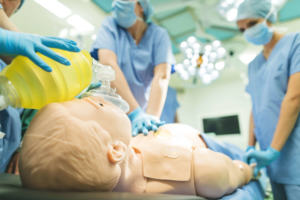
Laparoscopic simulator boxes, Basic and Advanced Life Support courses, Suturing Skill Table, Airway and Emergency Simulator, etc. may include audio (like breathing or heart sounds, without the realism of the actually movement of the patient, voice etc. its focus is on a single complex task)
A CPR trainer can support a realistic teaching experience in the cardiopulmonary emergences and its management
HIGH FIDELITY
High fidelity is the most realistic simulation experience. We practise it in our HU Anatomy Lab on human specimens, and in our computer-based mannequins and realistic environments to mimic operating rooms, emergency wards or interventional departments in the HU Simulation Center.
High fidelity replicates the clinical setting, the operating room, the intensive care wards, the general patient management area and many more.

VIRTUAL REALITY
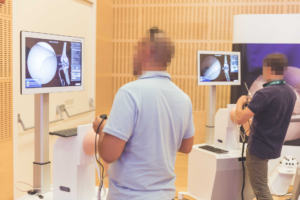
Virtual reality is a new field, which allows the operator to get a realistic practical feeling. Often used in the field of endoscopy and laparoscopy, where haptic feedback helps the operator to improve in the most realistic and dynamic way.
The arthroscopy trainer provides realistic haptic feedback to effectively understand action and effects.
SOFT SKILLS
Interpersonal communication, teamwork, leadership, decision-making, the ability to prioritize tasks under pressure, and stress management. Actors are trained to simulate scenarios like difficult conversations, family involvement, etc.
MAIN CHALLENGES
– Simulation is a replication of the real world, and should not be seen as a complete replacement of clinical training. Up to date, little is knows about the transferability of skills acquired through simulation into the clinical routine.
– Standardization: research is needed to define and optimize the methodology of simulation
Generally, simulation offers a huge opportunity to improve clinical skills, increase confidence of trainees, and ultimately improve patient care delivery. We are continuously engaging in research studies to understand the best mode of training delivery, and to optimize the way people can transfer the acquired skills into their daily clinical practice. A combination of research studies and in-situ quality improvement projects will help us understand the most realistic way to deliver clinical training.